Where does it come from?
Suitable for
Advantages of nebulized inhalation therapy
Therefore, nebulized inhalation drug delivery has the following advantages:
Particle settling
Commonly used nebulized inhalation drugs
Inhaled glucocorticoids ICS: budesonide (BUD) and beclomethasone propionate (BDP)
Bronchodilators: short-acting selective β2 agonists (SABA), including terbutaline and salbutamol;
Short-acting cholinergic receptor antagonists (SAMA): ipratropium bromide
Antimicrobials: tobramycin inhalation solution
Expectorants: including N-acetylcysteamine and Ambroxol hydrochloride
Where does it come from?
Case study children with PCD in the community of Madrid, Spain, have shown significant improvement with Feellife's AirKids professional medical-grade nebulizer. Nebulized inhalation treatments are fast-acting and highly compliant, requiring no patient intervention, which facilitates the long-term treatment of children using the device. Children with PCD in the community of Madrid, Spain, have shown significant improvement with Feellife's AirKids professional medical-grade nebulizer. Nebulized inhalation treatments are fast-acting and highly compliant, requiring no patient intervention, which facilitates the long-term treatment of children using the device.
About Lung Health Management
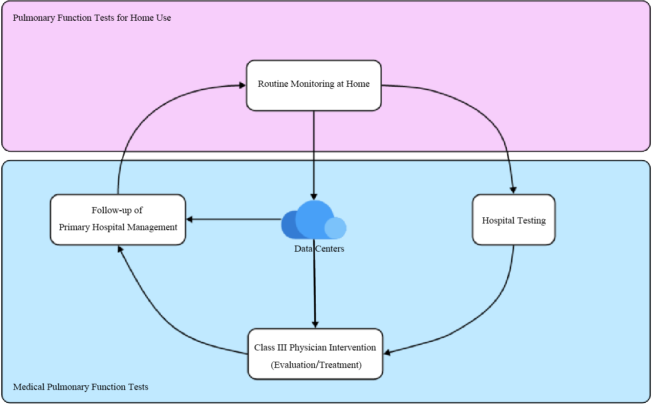
Pulmonary Function Tests
The Role of Lung Function Tests
Pulmonary Rehabilitation
The American Thoracic Society (ATS) and the European Respiratory Society (ERS) state:
Pulmonary rehabilitation is a comprehensive intervention based on an in-depth assessment of the patient after individualized treatment, including but not limited to exercise training, education, and behavioral change, with the goal of improving the physical and psychological status of the chronic respiratory patient and adherence to improved health behaviors over time. It can reduce clinical symptoms, optimize functional status, increase participation rates and reduce disease-related healthcare expenditures.
Pulmonary rehabilitation improves pulmonary function and psychological status, improves quality of life, enhances social adaptation, and reduces hospitalizations and morbidity and mortality.
The GLOD guideline suggests that COPD patients should perform moderate-intensity activity exercise for 6-24 min per day or 150 min per week, including respiratory training (breathing pattern training, inspiratory muscle training, and sputum expectoration training), aerobic exercise (e.g., brisk walking, bicycling, and jumping rope, etc.), strength training, and balance training, etc.
Where does it come from?
Case Study Feellife, in conjunction with the Kuur Clinic, is supporting the Dubai Professional Rugby Club with specialized medical equipment. The Airfit1 Breathing Trainer will increase the oxygen intake capacity of the JebelAliDragons Club athletes during long training sessions, improving endurance and rapid recovery of muscles, helping to cope with high-intensity matches and reducing the risk of injury. Feellife, in conjunction with the Kuur Clinic, is supporting the Dubai Professional Rugby Club with specialized medical equipment. The Airfit1 Breathing Trainer will increase the oxygen intake capacity of the JebelAliDragons Club athletes during long training sessions, improving endurance and rapid recovery of muscles, helping to cope with high-intensity matches and reducing the risk of injury.


