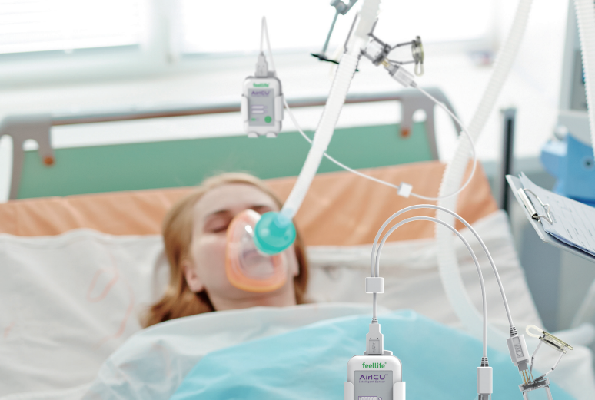
What is Noninvasive Positive Pressure Ventilation? (NIPPV)
(non-invasive positive pressure ventilation, NIPPV)
A technique that does not require invasive or invasive tracheal intubation or tracheotomy, but simply connects the patient to a ventilator for positive pressure assisted ventilation by means of a nasal mask, nasal-oral mask, full face mask, or headgear. It can open the collapsed upper airway to some extent, improve lung ventilation volume, improve ventilation and ventilation/blood flow ratio, improve oxygenation and carbon dioxide retention.
In the past 30 years, with the deepening of clinical research and practice of NIPPV, it has not only been confirmed that NIPPV is efficacious, can improve the survival rate of patients, avoid a series of complications brought about by invasive mechanical ventilation, and reduce the cost of treatment, but also is easy to implement and accepted by the patients, and has become a means of ventilation support in the early stage of pathophysiological states such as respiratory failure and in emergency situations.
Continuous positive airway pressure (CPAP)
It refers to the continuous positive pressure support given by the ventilator at the same level throughout the respiratory cycle under the condition of patient’s voluntary respiration, assisting the patient to complete all the respiratory movements. During inspiration, positive pressure is beneficial to overcome airway resistance and reduce the work done by the respiratory muscles; during expiration, positive pressure in the airway prevents small airway trapping, increases the functional residual air volume, and improves oxygenation.
In addition, the positive chest pressure generated by CPAP, which reduces return blood volume (preload) is beneficial for the combined effect in patients with acute cardiogenic pulmonary edema, but too much CPAP may be harmful in patients who already have a significant reduction in cardiac output.
Bi-level positive airway pressure (BIPAP)
BIPAP is a time-switching-pressure-controlled mode of mechanical ventilation that regulates inspiratory positive airway pressure (IPAP) and expiratory positive airway pressure (EPAP) separately and is an extension of the CPAP mode. The CPAP model is an extension of IPAP.
According to the mechanism of inspiratory-expiratory transition, BIPAP can be categorized into spontaneous (S) ventilation-assisted mode, time-controlled (T) mode, and spontaneous ventilation-assisted combined with time-controlled (S/T) mode.
Assured average volume pressure support (AVAPS)
AVAPS is a hybrid ventilation mode whose basic principle remains pressure support. To achieve a predetermined ventilatory tidal volume, inspiratory pressure is set at a range interval rather than a fixed value. The ventilator automatically adjusts IPAP to achieve the predetermined ventilatory tidal volume based on the measured ventilation volume.
Typically, increasing CPAP and EPAP levels helps to improve hypoxia and maintain upper airway opening; increasing the difference between IPAP and EPAP or increasing the ventilation volume helps to improve alveolar ventilation, increase CO2 efflux, and reduce inspiratory work done by the patient.
Why Choose The Air ICU Series?
Experiments have demonstrated that the mesh nebulizer is currently the most ideal nebulizing device for delivering inhaled preparations for use in conjunction with a ventilator.
Compared to compression nebulizers, mesh nebulizers have a higher delivery efficiency than compression nebulizers when used in conjunction with a ventilator [1].
Compared to ultrasonic nebulizers, ultrasonic nebulizers have been used less frequently in clinical practice due to the inability to nebulize viscous solutions, the potential for the heat generated to destroy the solution, and larger residues [2].
Compared to pMDI and due to difficulty in synchronizing inhalation, pMDI reduces drug delivery and drug dose may change due to separation from the ejection agent [3].
Air ICU is a new generation of professional mesh nebulizer with feellife core patents
It is embedded with AiMesh®inside polymer diaphragm technology and breath sensing technology
[1] Berlinski A and Willis JR. Albuterol delivery by 4 different nebulizers placed in 4 different positionsin a pediatric ventilator in vitro model. Respiratory care.2013,58:1124-33.
[2] Ari A and Fink JB. Guidelines for aerosol devices in infants, children and adults: which to choose, why and how to achieve effective aerosol therapy. Expert review of respiratory medicine.2011;5:561-72.
[3] Diot P, Morra Land Smaldone GC. Albuterol delivery in a model of mechanical ventilation. Comparison of metered-dose inhaler and nebulizer efficiency. American journal of respiratory and critical care medicine.1995;152:1391-4.
